Do you often find yourself dealing with itchy, irritated skin? If so, you might be one of the millions of people worldwide who suffer from eczema. However, have you ever wondered where on your body you are most likely to experience this frustrating skin condition? From the sensitive skin of your face to the folds of your elbows and knees, this article will explore the different areas where eczema commonly occurs, helping you better understand and manage this pesky condition. So, let’s dive in and discover where you are most likely to get eczema!
Common Areas for Eczema
Face and Neck
Eczema can commonly occur on the face and neck, causing redness, itching, and dryness. The sensitive skin in these areas is more prone to flare-ups, especially around the eyes and mouth. Factors like harsh skincare products, weather changes, and allergens can trigger eczema on the face and neck.
Hands
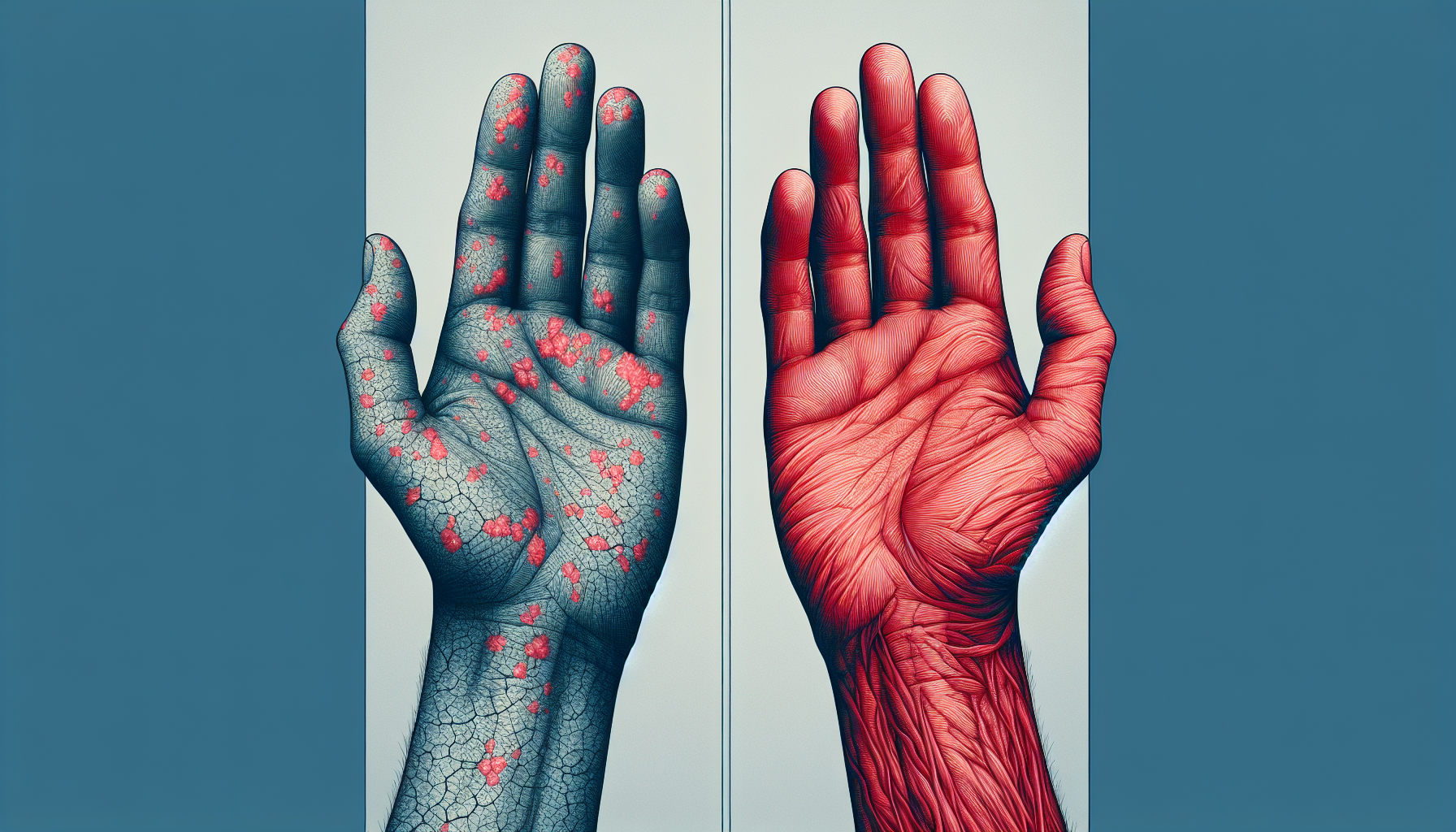
The hands are frequently exposed to various irritants and chemicals, making them highly susceptible to eczema. Activities such as washing dishes, using cleaning products, or handling certain materials can trigger eczema on the hands. Symptoms may include dry, cracked, and itchy skin.
Elbows and Knees
Eczema often appears on the elbows and knees due to the frequent bending and rubbing of these joints. The skin in these areas can become dry, scaly, and inflamed. Friction from clothing, excessive sweating, and harsh weather conditions can also contribute to eczema flare-ups.
Behind the Ears
The skin behind the ears is thin and delicate, making it prone to eczema. Factors like heat, excessive moisture, and allergens can cause red, itchy rashes in this area. Additionally, certain hair products or earrings may contain substances that can irritate the skin behind the ears.
Wrists
Eczema can affect the wrists, leading to itching, redness, and dryness. The constant movement of the hands and exposure to water or chemicals can contribute to eczema flare-ups in this area. Wearing tight wristbands, bracelets, or watches can also further aggravate the skin.
Ankles
The ankles are a common site for eczema, particularly due to the friction from shoes and socks. Additionally, sweat and heat can accumulate in this area, creating a moist environment that triggers eczema flare-ups. It is essential to wear breathable footwear and avoid tight socks to prevent irritation.
Feet
Eczema can appear on the feet, causing discomfort and itchiness. This can be attributed to wearing closed shoes for long durations, excessive sweating, or exposure to irritants like certain fabrics or chemicals. Maintaining good foot hygiene, wearing breathable shoes, and using moisturizers can help manage foot eczema.
Genital Area
Although less common, eczema can occur in the genital area. This may be due to moisture, sweat, friction, or the use of certain personal care products. It is important to seek medical advice and avoid self-treatment in this sensitive area to prevent further complications.
Eyelids
Eczema on the eyelids can be particularly bothersome and can cause redness, itching, and swelling. Factors like allergies, cosmetics, or rubbing the eyes can trigger eczema in this area. It is crucial to avoid using harsh eye makeup products and to seek medical guidance for proper treatment.
Scalp
Eczema on the scalp can lead to dandruff-like flakes, itchiness, and inflammation. Factors such as dry skin, sensitivity to hair products, or certain skin conditions can contribute to scalp eczema. Gentle cleansing with mild shampoos, avoiding hot water, and moisturizing the scalp can help manage this condition.
Environmental Factors that Influence Eczema
Climate and Weather Conditions
The climate and weather can significantly impact eczema symptoms. Cold weather can strip the skin of moisture, leading to dryness and flare-ups. Similarly, hot and humid weather can cause excessive sweating and irritation. It is important to protect your skin from extreme weather conditions and adjust your skincare routine accordingly.
Indoor Air Quality
Indoor air quality plays a crucial role in triggering or exacerbating eczema. Dry air, dust, pet dander, and mold can all irritate the skin and worsen eczema symptoms. Proper ventilation, regular cleaning, and using humidifiers or air purifiers can help improve indoor air quality and minimize eczema triggers.
Chemicals and Irritants
Exposure to harsh chemicals and irritants can trigger eczema flare-ups. Cleaning products, such as detergents and soaps, may contain ingredients that irritate the skin. Similarly, certain fabrics, fragrances, or skincare products can also cause eczema reactions. It is crucial to choose hypoallergenic and fragrance-free options and wear protective gloves when handling irritants.
Allergens
Allergens play a significant role in eczema reactions. Common allergens include pollen, dust mites, pet dander, and certain foods. Avoiding exposure to known allergens, practicing good hygiene, and seeking medical advice to identify specific allergens can help manage and prevent eczema flare-ups.
Clothing and Fabrics
Wearing certain fabrics or tight clothing can aggravate eczema. Rough or synthetic materials can cause friction, leading to itchiness and irritation. Opting for soft, breathable fabrics such as cotton and avoiding tight-fitting clothing can help reduce eczema symptoms.
Lifestyle and Personal Habits
Skin Care Routine
Establishing a suitable skincare routine is essential for managing eczema. Using gentle, non-irritating cleansers, moisturizing regularly, and avoiding hot water can help soothe and protect the skin. Applying topical corticosteroids or prescribed medications as directed by a healthcare professional can also be part of an effective skincare routine.
Hygiene Practices
Maintaining good hygiene practices is vital for managing eczema. Taking lukewarm showers or baths instead of hot ones, using mild soaps and cleansers, and patting dry the skin can prevent excessive drying and irritation. Avoiding frequent scrubbing and opting for gentle skincare practices can help minimize eczema flare-ups.
Physical Activities
Engaging in physical activities can have both positive and negative effects on eczema. Sweating during exercise can trigger flare-ups, but incorporating relaxation techniques and low-impact activities like yoga or swimming can help reduce stress levels and promote overall well-being. It is important to find a balance and listen to your body’s needs.
Occupational Exposure
Healthcare Workers
Healthcare workers, including nurses and doctors, are frequently exposed to various irritants and allergens that can trigger eczema. Frequent handwashing, wearing gloves, and exposure to healthcare-related chemicals can contribute to eczema flare-ups. Proper personal protective equipment, regular moisturization, and selecting suitable skincare products are crucial for managing eczema in this profession.
Hairdressers and Beauticians
Hairdressers and beauticians often work with chemicals and hair products that can irritate the skin, leading to eczema. Frequent exposure to hair dyes, shampoos, and styling products, as well as constant handwashing, can trigger flare-ups. Using gloves, minimizing exposure to the chemicals, and practicing proper skincare can help minimize the risk of eczema in this occupation.
Construction Workers
Construction workers are exposed to various irritants, dust, and chemicals that can trigger eczema. Constant contact with construction materials, prolonged sweating, and friction from protective gear can contribute to flare-ups. Wearing suitable protective clothing, using gloves, and practicing good hygiene can help minimize eczema in this line of work.
Mechanics
Mechanics often come into contact with chemicals, solvents, and oils that can irritate the skin and trigger eczema. Prolonged use of soaps and hand cleansers can further dry out the skin, leading to flare-ups. Wearing protective gloves and using barrier creams, as well as practicing good hand hygiene, are essential for managing eczema in this profession.
Cleaners
Cleaners frequently use strong chemicals and cleaning agents that can cause skin irritation and eczema. The repetitive exposure to cleaning products, prolonged contact with water, and scrubbing can worsen eczema symptoms. Wearing gloves, using mild cleaning products, and moisturizing the skin after work can help protect against eczema flare-ups.
Age and Gender Factors
Infants and Children
Eczema is prevalent in infants and children, often appearing on the face, scalp, and extremities. The exact causes of childhood eczema are not fully understood, but factors such as genetics, allergens, and environmental triggers can contribute to its development. It is crucial to establish a gentle skincare routine, identify and avoid triggers, and seek medical advice for appropriate treatment in children with eczema.
Teenagers
Teenagers can experience eczema flare-ups on different parts of the body, including the face, neck, hands, and feet. Hormonal changes, stress, and environmental factors can trigger eczema in this age group. Practicing good skincare habits, managing stress levels, and seeking medical guidance for proper treatment can help teenagers manage their eczema effectively.
Adults
Eczema can persist into adulthood or develop later in life. Common areas for eczema in adults include the hands, wrists, and elbows. Stress, environmental factors, and genetics can contribute to eczema in this age group. Maintaining a consistent skincare routine, identifying triggers, and seeking medical advice are essential for managing eczema symptoms in adults.
Men vs. Women
Eczema can affect both men and women, although certain studies suggest a higher prevalence in women. Hormonal fluctuations, skincare routines, and clothing choices can play a role in eczema flare-ups in women. Men, on the other hand, may be more prone to occupational eczema due to exposure to irritants in certain professions. Personalized skincare routines and seeking professional advice can help both men and women effectively manage their eczema.
Genetic Predisposition
Family History
Eczema often runs in families, indicating a genetic predisposition. If a close family member, such as a parent or sibling, has eczema, there is an increased likelihood of developing it as well. Understanding the genetic component can help individuals take proactive measures to prevent or manage eczema effectively.
Ethnicity
Certain ethnicities have a higher prevalence of eczema. For example, individuals of African, Asian, and Caribbean descent may be more prone to eczema compared to other ethnic groups. This may be attributed to genetic factors and variations in skin barrier function. Recognizing these predispositions can aid in tailoring treatment plans to specific ethnic populations.
In conclusion, eczema can occur in various areas of the body, with some being more common than others. Factors such as genetics, environmental triggers, and lifestyle habits can all influence the development and severity of eczema. By understanding these common areas, environmental factors, personal habits, occupational exposure, age and gender factors, and genetic predisposition, individuals can take proactive steps to prevent and manage eczema effectively.